Brief context analysis and needs identification during Corona pandemic in Kenya and Nepal
While China, Europe and the United States are currently hit hard by the Corona crisis, there has been limited attention so far for the situation in low and middle-income countries (LMICs). Therefore, TU Delft Global Initiative created a short document with the aim of highlighting the current situation in Kenya and Nepal as we collaborate with these countries within our Healthcare for All Programme. Here we present some facts to get a deeper understanding of the local healthcare context and the current needs in the Covid-19 crisis.
Unfolding Situation
In recent weeks, daily life for many people has changed rapidly as more and more countries went into lockdown and the harsh reality of these measures for a large population in LMICs is highlighted in news outlets. Sub-Sahara Africa, South-East Asia, Latin America and the rest of the world are watching with bated breath on how the situation in these often fragile healthcare systems will evolve in the upcoming weeks and months.
Kenya and Nepal
DGI performed an in-depth exploration on the current situation in Kenya and Nepal, using online sources and short interviews with the healthcare and makerspace network we have in these countries. We found that there is a marked lack of personal protective equipment (PPE) for healthcare professionals, combined with a health system that was already operating on or over the maximum capacity before the pandemic. In addition, society is structured in such a way that working from home is nearly impossible for the majority of people, as their livelihood depends on their daily work. This further increases risk of contamination and deregulation of society.
Statistics on Covid-19 cases
The number of cases, though rising are still low compared to e.g. Europe and the US. Some interesting mechanisms could play a role here:
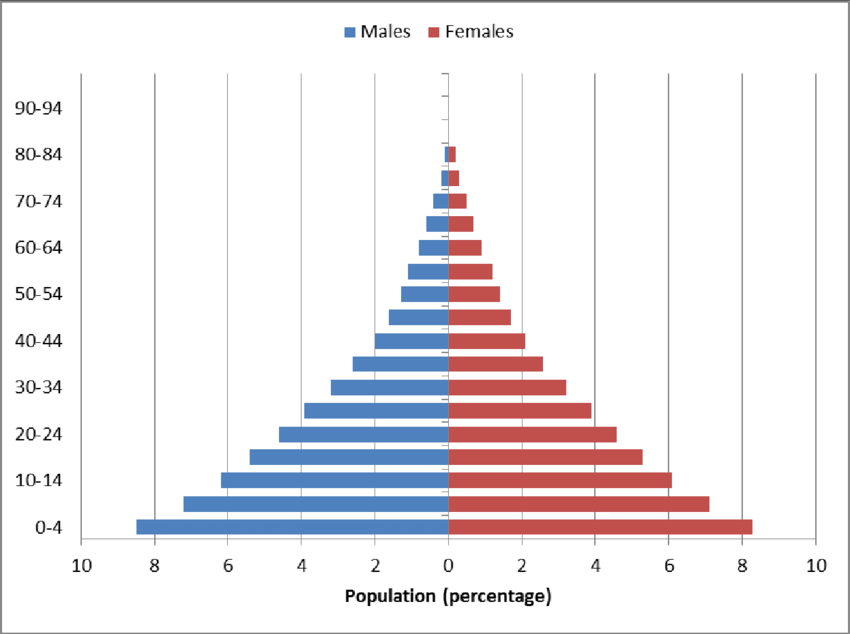
- The age pyramid. In Africa on the whole, there are relatively few people in the affected age groups.
- Testing capacity is low. Because of this, there is no real way of knowing how many people exactly have been infected.
- Sub-Saharan Africa appears to be affected after China, Europe and US, and therefore has a delay in cases.
However, there are also still concerns and unanswered questions. 70 % of African urbanites—approximately 200 million people—reside in crowded city slums. 40 % of Africans live in water-stressed environments in which obtaining access to clean water—let alone soap is very challenging. And for the 85 % of Africans who live on less than $5.50 per day, work stoppages will pose a threat to their daily lives. Finally, a major unanswered question is how malnutrition, HIV-AIDs, tuberculosis, malaria, or other chronic conditions will interact with COVID-19.
Recommendations
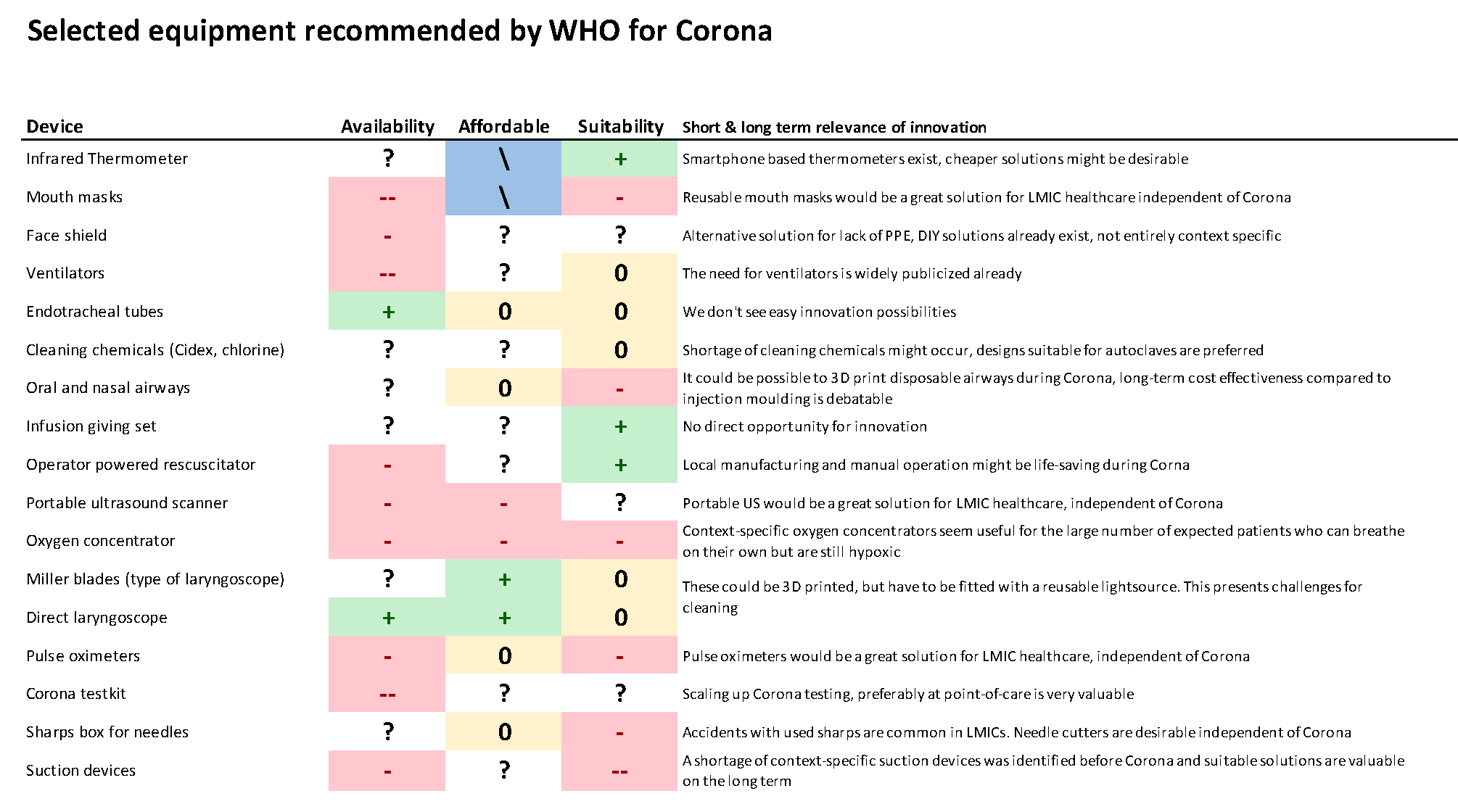
The World Health Organisation (WHO) has provided a list of equipment required during the Corona pandemic called the Operational Support & Logistics Disease Commodity Packages (DCP-NCOV). Equipment designed for use in high-income countries is not always suitable for use in low-resource regions. The report includes a table detailing the suitability of each recommendation for usage in low-resource regions, as well as subjective recommendations concerning the possible impact of creating context-specific variants of these devices.
As quickly becomes apparent, while many of the devices would certainly aid combatting the corona crisis, on the whole they are not widely available, affordable, or suitable for low-resource regions. TU Delft | Global Initiative works together with Guatemala in testing an affordable, locally producible respirator in the Project Inspiration initiative. The TU Delft | Global Initiative will also work together with KNUST in Ghana and Oregon State University on helmet-based ventilation. These initiatives will work towards better matching corona-related needs of those regions through achievable means.
Download and read the report in full here
(with thanks to Roos Oosting, Julie Fleischer and Karl Heinz Tondo)
Contact
Dr. ir. Jan-Carel Diehl
j.c.diehl@tudelft.nl