Talking the walk: tailored healthcare
Hospitals want happy and satisfied patients. And they need them, because healthcare is a competitive market. Especially when it comes to non-life threatening procedures, public hospitals face serious competition from private clinics, where there is an increasing focus on the patient experience, or the ‘patient journey’ as it is called. But how do you create the right patient experience and good, manageable tailored care? Bob Groeneveld researched this question using one common procedure as an example: a total hip replacement.
What do you want?
The non-life threatening and often pre-planned nature of a hip replacement made it perfect for his research. Groeneveld: ‘During this procedure, patients are often seen more as customers. They sometimes have high expectations for these kinds of planned procedures. This makes managing expectations beforehand a little easier. Patient satisfaction is dependent on how expectations are subsequently met by the hospital or clinic.’ ‘You already have a lot of tailored digital communication’, Groeneveld explains. ‘There are online decision making tools, which take you step-by-step through the process of deciding if hip-surgery is right for you. And you have websites that give information for patients with special conditions such as diabetes or obesity. But, as Groeneveld says, you want the communication to be tailored to the specific information need of the patient.’
To develop this, his project partner and psychologist Tessa Dekkers took a pool of variables as a starting point. How do people experience their health? Do they feel stressed before surgery? The goal of Groeneveld and Dekkers was to segment into sub-divisions which could form a basis for tailored information. After a large-scale research project, three main groups emerged: optimistic, controlling and modest patients.
Design your own journey
The next step was a smaller-scale piece of research with the aim of delivering a theoretical model. Groeneveld developed paper prototypes to help do this. These took the form of a sort of diary in which people could collect and share information. Groeneveld: “Storyboards also gave people a chance to voice their opinion without needing to design an entire website.’ They also organised so-called generative sessions, where participants were actively involved in the design. ‘We let them think about the ideal patient experience’, Groeneveld says. ‘They made collages about it. The stories people reveal interesting information about what they feel is important.’ This stage in the research led to a more granular division of the groups. For instance, the people that wanted control felt the need for a lot of information during the rehabilitation process. But what that means, differs a lot depending on the situation, Groeneveld explains. ‘One person might want to go skiing as soon as possible, while another wants to be able to pick up their grand-daughter.’
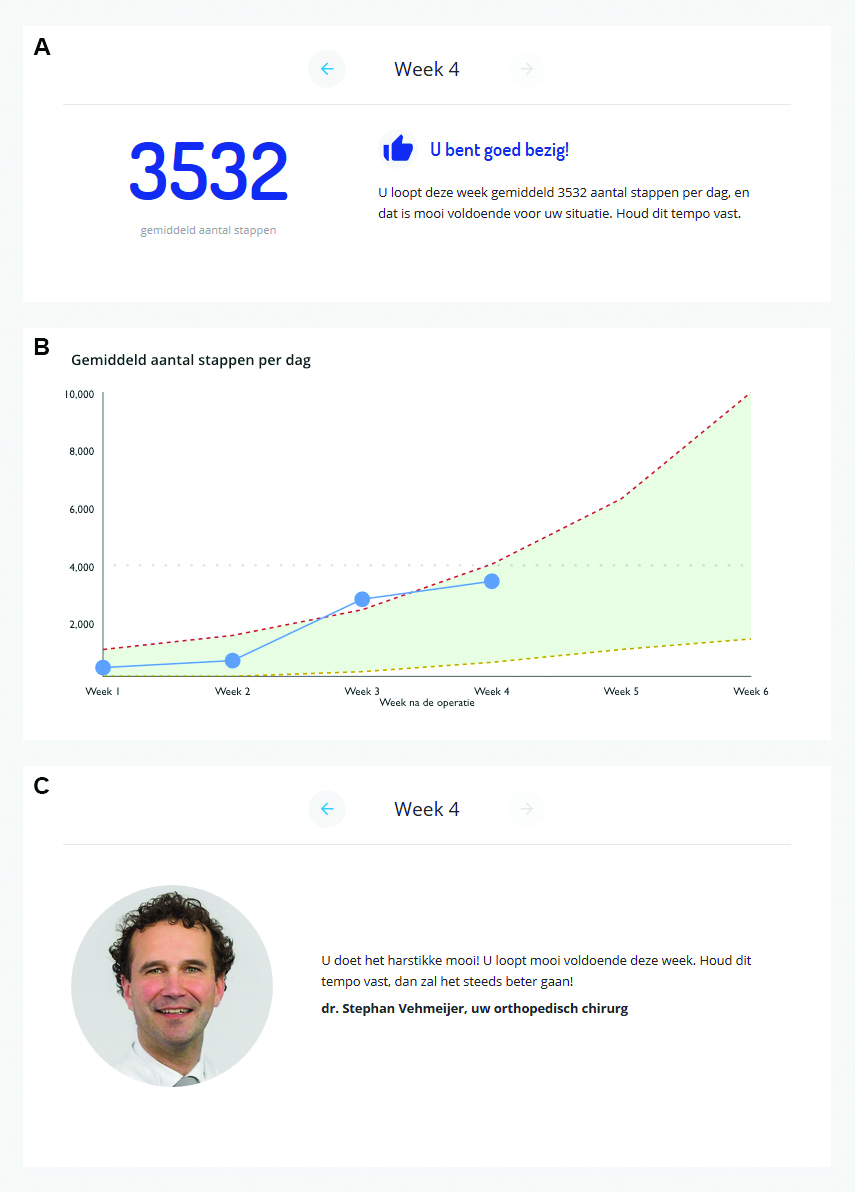
Twenty patients from the research went on to test a web application designed by Groeneveld. Optimistic patients were deliberately excluded from this exercise. A logical choice, as these patients seldom experience stress through the treatment process and therefore rarely require extra support. The application which includes a step-counter, an information exchange option and a rehabilitation walking schedule, offers insight and support for about half of the target audience of hip-replacement surgery patients.
Big pressure and small gestures
Supporting half of the patients sounds like a good start, but Groeneveld realises that tailored healthcare in practice is a balancing act. It’s a case of navigating between added value for patients and manageability for healthcare professionals. Improvements in patient experiences require more effort by healthcare workers. But there is already a great deal of pressure on these workers. Groeneveld offers a small, nuanced bit of commentary to his research: ‘The quality of care is often showcased by the little things healthcare workers do. Things that make patients think: there is somebody here with me, who cares about me.’ Small gestures can have a big impact. Groeneveld: ‘One patient told me that he had a hemorrhage right after surgery, an unexpected complication. The orthopedist surgeon ran to the recovery unit in between two different appointments to check on the patient. That patient really appreciated that extra effort.’
Whatever healthcare model is put in place, what Groeneveld is saying is that we always need to hold on to our shared humanity.

Richard Goossens
- +31 (0)15 27 86340
- R.H.M.Goossens@tudelft.nl
-
Room C-3-140
"In the end there is a solution for everything."
Marijke Melles
- +31 (0)15 27 87514
- M.Melles@tudelft.nl
-
Room C-3-080
"A well thought-out medical product reflects the daily experiences of the medical practitioner."