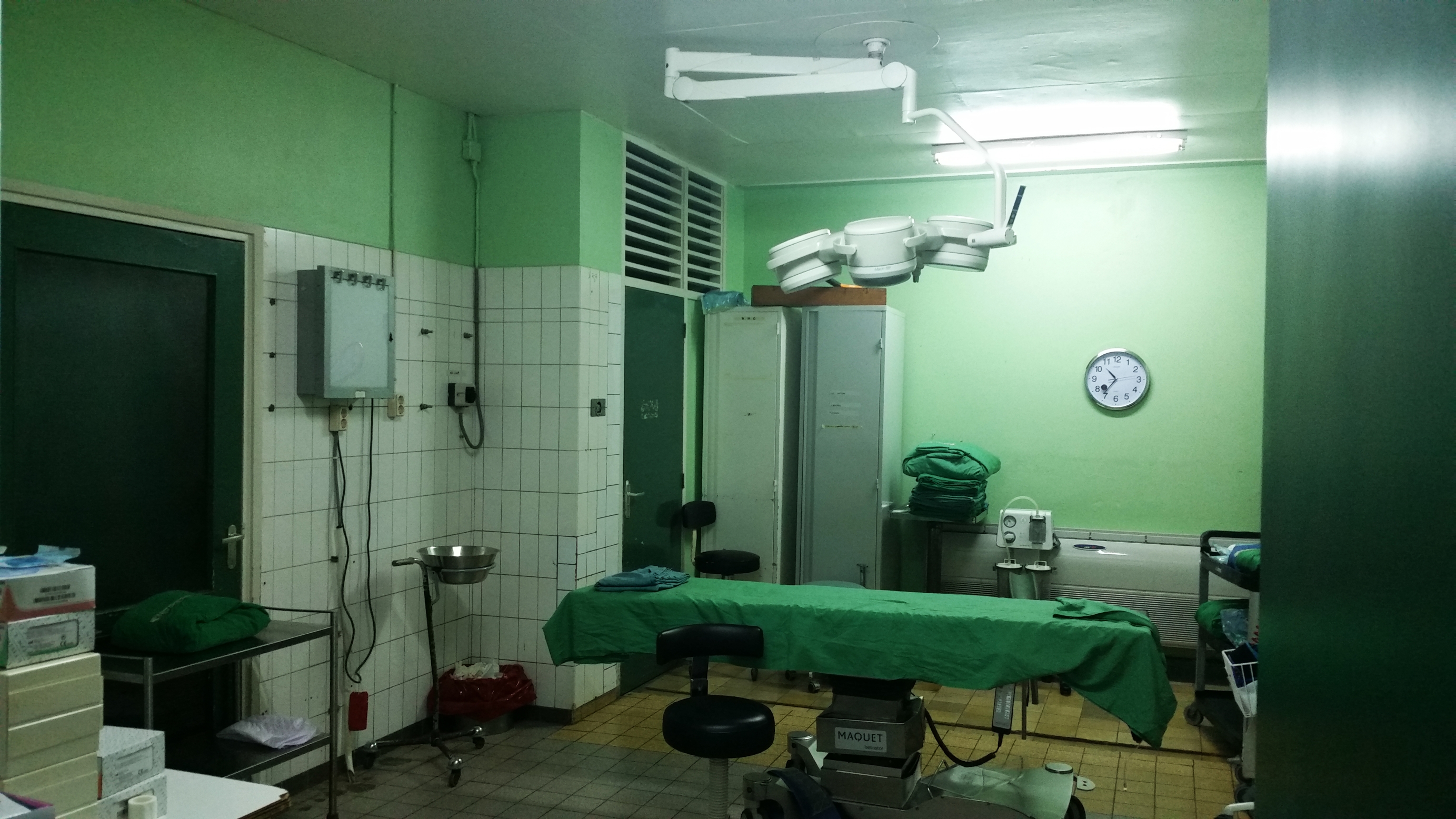
We’ve all been there. You have had an accident, perhaps bruised or broken a limb. Off you go to the accident and emergency department at the hospital. In Africa things are not quite that straightforward. 85% of all 15 year-olds who needed a minor or more important surgical intervention at one point did not get it. Treatment, if available at all, is often at a couple of days travel. Often that is simply too long and patients are left with impairments varying from minor to life-changing, or even die. Worldwide a lack of access to basic healthcare kills more people than malaria, HIV/aids and tuberculosis put together. That is why Jenny Dankelman’s TU Delft Global project is all about developing safe and affordable surgical instruments.
One of the most complex surgical instruments is an electrosurgical device used to make incisions and cauterise wounds. After cutting, blood loss is kept to a minimum by cauterising the wound as quickly as possible. “Even for highly trained doctors it’s not the easiest of instruments. It has different settings for cutting and cauterising. Research shows that surgeons don’t always know exactly what the different settings mean. As a result, the device is sometimes used inappropriately and that can have serious consequences.” These devices also find their way to hospitals all over the world.
Focus on the device
Clinical surgery departments have been involved in numerous efforts to raise funds for training local surgeons. “But I prefer to focus on the device, not the person who’s using it. Why not make the device easier to use? That is how my group works: we try to find simple solutions. Moreover, apart from use, maintenance, the replacement of parts and an unstable electricity supply can also be a problem in hospitals in low-and middle-income countries. Robot technology is a hot topic in Dankelman’s field of expertise. “That kind of technology is not always the best way forward. For maximum impact you want to keep things affordable and simple, especially in low-and-middle income countries where healthcare budgets are very limited. And that is what we are aiming for in this TU Delft Global Research Fellowship.” Dankelman projected development time for a fast, compact and reliable device is four years. This device will be user-friendly and will continue to work during power outages.
Working together
For Dankelman, collaboration is key. “I am a complete novice when it comes to doing work in low- and middle-income countries. Luckily, I am learning from working together with partners within and outside of TU Delft.” Dankelman studies the context in which surgical equipment is used in Sub Saharan Africa together with experts in Biomechanical engineering from Kenyatta University in Nairobi, Kenya. “And Diamedica is a commercial partner in our project. They have experience in building medical equipment for several low- and middle-income countries.” PhD researcher Roos Oosting together with TU Delft colleague J.C. Diehl from the department of Industrial Design explores the user interface and training for hospitals in Sub Saharan Africa. Oosting: “Master students from Industrial Design already investigated the medical device journey in Kenya. They set up requirements for the electrosurgical device, including the user interface.”
Minimally invasive surgery
This TU Delft Global project is only the start, Dankelman says. As professor of Minimally Invasive Surgery and Intervention Techniques she knows all there is to know about operating through small holes, or ‘keyhole surgery’ as it is popularly known. Using smart instruments, needles and flexible catheters, incision size can be brought back considerably, keeping the risk of infection to a minimum. Dankelman’s goal is to start several projects around the improvement of surgical instruments for hospitals in low-and middle-income countries. “I would start with instrument and operating room sterility issues. But ultimately I would like to take the step from open surgery to minimally invasive surgery.”