Breathing (more) easily through aerospace engineering
A team of researchers, led by Prof. Leroux at ETH Zürich, have developed a new personalized biodegradable 3D printed stent for the windpipe. For this they used a new polymer chemistry and a light based 3D printer that works at high temperatures, making it possible to produce stents that exactly match the anatomy of the patient. Operations to remove stents – risky especially in older patients and children – can be prevented as the stent will degrade over time. The scientific publication of the group, including researcher Kunal Masania of the faculty of Aerospace Engineering TU Delft, is published today in Science Advances.
Tissue damage
Central airway obstruction (CAO) is a life-threatening disorder, caused for example by lung cancer, for which patients need to be intubated. Currently, the stents used for the stenosis provoked by intubation are made of metal or silicone, and are available in a limited number of sizes and shapes. Ill-fitting stents can, however, move around in the windpipe, causing damage to the tissue. After treatment, the stents need to be removed surgically, risking further tissue damage. This is especially critical in children whose airways are still growing or in elderly or medically fragile patients.
An international group of researchers, led by Prof. Leroux of the Institute of Pharmaceutical Sciences, Department of Chemistry and Applied Biosciences, ETH Zürich, researched the option of developing stents that could be 3D printed to match the exact anatomy of the patient and that could biodegrade over time, making operations unnecessary.
Aerospace grade 3D printing of materials
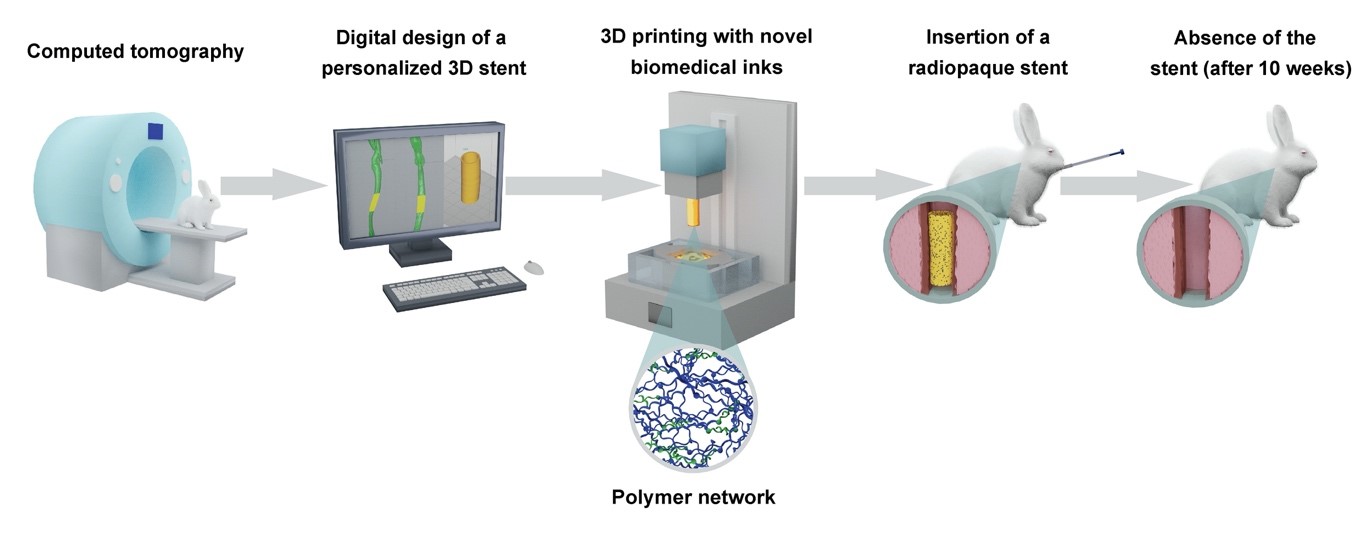
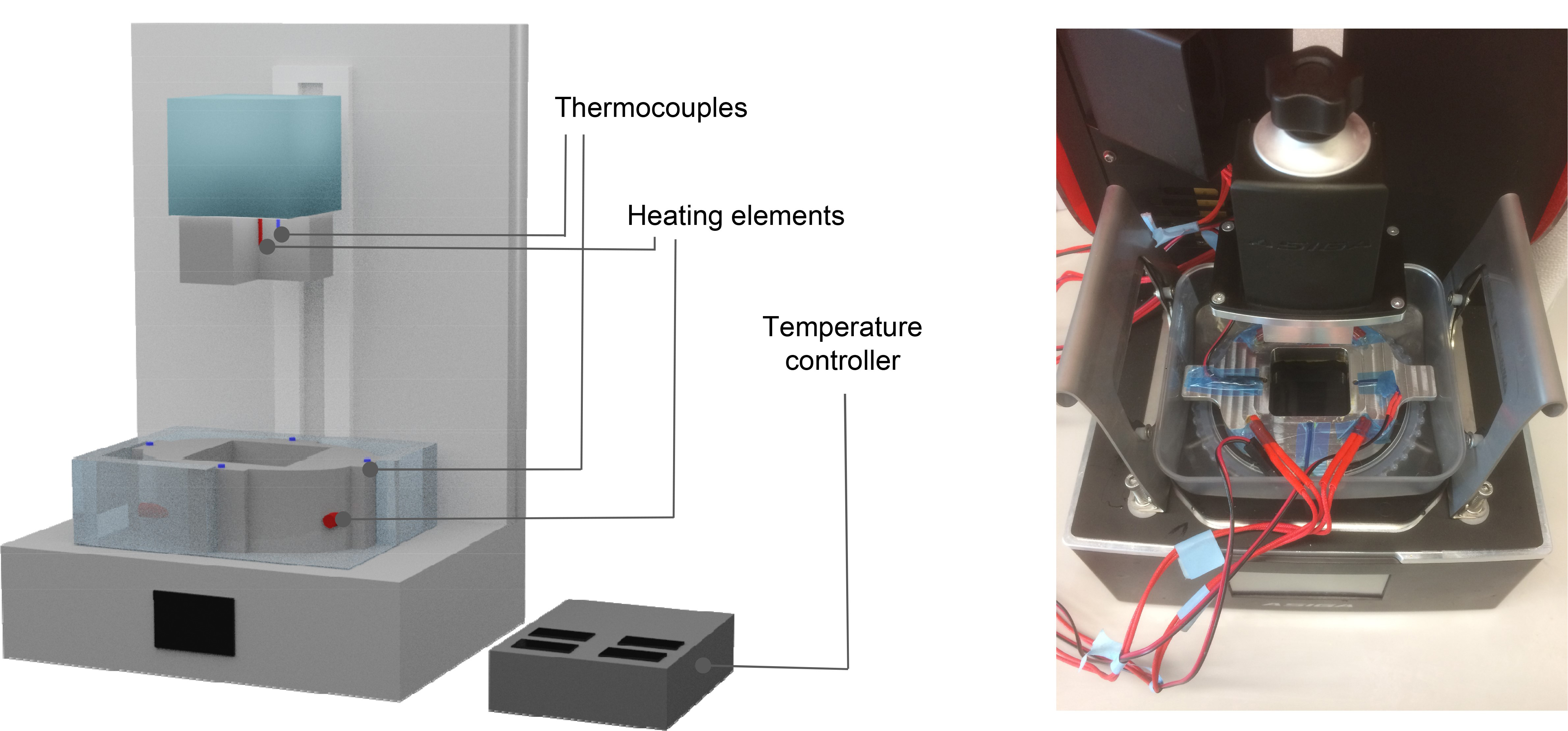
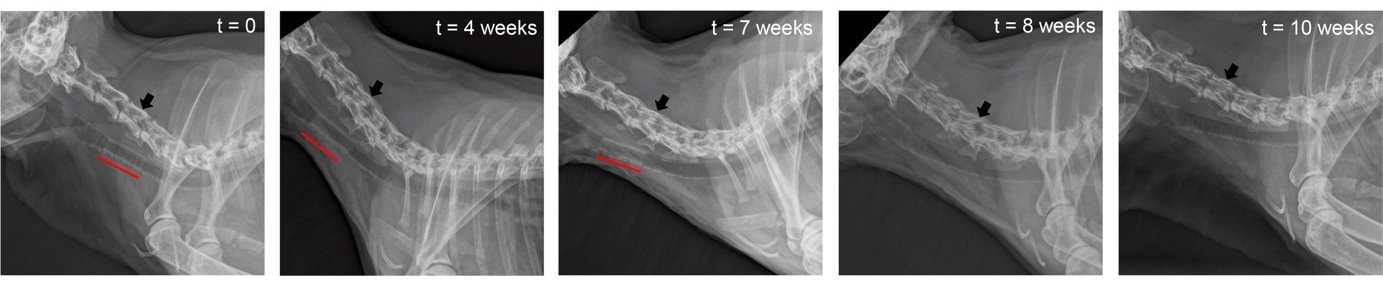
For this, they turned to aerospace engineering. Kunal Masania, previously in Prof. Studart’s Complex Materials Group at ETH Zürich, now Associate Professor at the faculty of Aerospace Engineering TU Delft: “The most suitable 3D printing technique for biomedical applications like stents is digital light processing (DLP), but its use is fairly limited because of a lack of suitable biodegradable inks. The current inks produce rigid and brittle objects that are not suitable for stents.” Together they developed a custom DLP printer capable of heating up to 200 C, a temperature typically associated with aerospace grade materials. This dramatically reduced the viscosity. In the end printing took place at temperatures of 70-90 C. Masania: “By combining the biodegradable ink with computed tomography, we successfully DLP 3D printed customized airway stents of high resolution, beyond what has been shown so far.” The stents were designed to degrade in the body after it has fulfilled its biomechanical function. When inserted into rabbits it disappeared after 7 weeks, without causing any permanent tissue damage or other side effects.
Alleviating breathing difficulties
This new technology enables fast and personalized treatment of patients suffering from CAO, alleviating breathing difficulties rapidly, without the need for additional surgeries. The team is further developing new compositions to fully unlock the potential of their findings. In his work at TU Delft, Masania will continue to focus on applying innovative aerospace materials manufacturing for societal impact in other extreme environments whether in Space or the human body.
Publication
The paper “Digital light 3D printing of customized bioresorbable airway stents with elastomeric properties” by Nevena Paunović, Yinyin Bao, Fergal Brian Coulter, Kunal Masania, Anna Karoline Geks, Karina Klein, Ahmad Rafsanjani, Jasmin Cadalbert, Peter W. Kronen, Nicole Kleger, Agnieszka Karol, Zhi Luo, Fabienne Rüber, Davide Brambilla, Brigitte von Rechenberg, Daniel Franzen, André R. Studart and Jean-Christophe Leroux appears today in the Journal Science Advances.
More information
Kunal Masania, Associate Professor, Shaping Matter Lab, Aerospace Manufacturing Technologies, TU Delft. Tel: +31 (0) 15 278 2774, K.Masania@tudelft.nl.
Ineke Boneschansker, communication manager Aerospace Engineering TU Delft. Tel: +31 (0) 15 278 5361, I.Boneschansker@tudelft.nl.
More information on the Shaping Matter Lab can be found here: www.shapingmatterlab.com
The team are most grateful to the Swiss National Science Foundation (project No. 177178) for supporting this Sinergia project for interdisciplinary, collaborative breakthroughs.